The liver is a
vital organ present in
vertebrates
and some other animals. It has a wide range of functions, including
detoxification,
protein synthesis, and production of biochemicals necessary for
digestion.
The liver is necessary for survival; there is currently no way to compensate for
the absence of liver function in the long term, although new
liver dialysis techniques can be used in the short term.
This
organ plays a major role in
metabolism
and has a number of functions in the body, including
glycogen
storage, decomposition of red blood cells,
plasma protein synthesis,
hormone
production, and detoxification. It lies below the diaphragm in the
abdominal-pelvic region of the abdomen. It produces
bile, an alkaline
compound which aids in
digestion
via the
emulsification of
lipids. The liver's highly specialized
tissues regulate a wide variety of high-volume biochemical reactions,
including the synthesis and breakdown of small and complex molecules, many of
which are necessary for normal vital functions.[2]
Terminology related to the liver often starts in hepar- or hepat-
from the
Greek word for liver, hēpar (ἧπαρ, root hepat-, ἡπατ-).
Anatomy
The liver is a reddish brown organ with four
lobes of unequal size and shape. A human liver normally weighs 1.44–1.66 kg
(3.2–3.7 lb),[3]
and is a soft, pinkish-brown, triangular organ. It is both the largest internal
organ (the skin
being the largest organ overall) and the largest
gland in the
human body. It is located in the
right upper quadrant of the
abdominal cavity, resting just below the
diaphragm. The liver lies to the right of the stomach and overlies the
gallbladder. It is connected to two large
blood
vessels, one called the hepatic artery and one called the
portal vein. The
hepatic artery carries blood from the aorta, whereas the portal vein carries
blood containing digested nutrients from the entire
gastrointestinal tract and also from the
spleen and
pancreas.
These blood vessels subdivide into capillaries, which then lead to a lobule.
Each lobule is made up of millions of hepatic cells which are the basic
metabolic cells.
Lobules are the functional units of the liver.
Cell types
Two major types of cells populate the liver lobes: karat parenchymal and
non-parenchymal cells. 80% of the liver volume is occupied by
parenchymal cells commonly referred to as
hepatocytes. Non-parenchymal cells constitute 40% of the total number of
liver cells but only 6.5% of its volume.
Sinusoidal hepatic endothelial cells,
Kupffer cells and
hepatic stellate cells are some of the non-parenchymal cells that line the
liver sinusoid.[4]
Blood flow
The liver gets a dual blood supply from the
hepatic portal vein and
hepatic arteries. Supplying approximately 75% of the liver's blood supply,
the hepatic portal vein carries
venous
blood drained from the
spleen,
gastrointestinal tract, and its associated organs. The hepatic arteries
supply arterial blood
to the liver, accounting for the remainder of its
blood flow.
Oxygen is provided from both sources; approximately half of the liver's oxygen
demand is met by the hepatic portal vein, and half is met by the hepatic
arteries.[5]
Blood flows through the
liver sinusoids and empties into the central vein of each lobule. The
central veins coalesce into hepatic veins, which leave the liver.

axial CT image showing anomalous hepatic veins coursing on the
subcapsular anterior surface of the liver.
[6]

Maximum intensity projection (MIP) CT image as viewed anteriorly
showing the anomalous hepatic veins coursing on the anterior surface
of the liver

Lateral MIP view in the same patient
Biliary flow
The term
biliary tree is derived from the arboreal branches of the bile ducts.
The bile produced
in the liver is collected in
bile canaliculi, which merge to form
bile ducts.
Within the liver, these ducts are called intrahepatic (within the liver)
bile ducts, and once they exit the liver they are considered extrahepatic
(outside the liver). The intrahepatic ducts eventually drain into the right and
left
hepatic ducts, which merge to form the
common hepatic duct. The
cystic
duct from the
gallbladder joins with the
common hepatic duct to form the
common bile duct.
Bile either drains directly into the
duodenum
via the common bile duct, or be temporarily stored in the
gallbladder via the cystic duct. The common bile duct and the
pancreatic duct enter the second part of the duodenum together at the
ampulla of Vater.
Surface anatomy
Peritoneal ligaments
Apart from a patch where it connects to the
diaphragm (the so-called "bare
area"), the liver is covered entirely by
visceral
peritoneum,
a thin, double-layered
membrane
that reduces
friction against other organs. The
peritoneum
folds back on itself to form the
falciform ligament and the
right and
left triangular ligaments.
These "lits"
are in no way related to the true
anatomic
ligaments in
joints, and have essentially no known functional importance, but they are
easily recognizable surface landmarks. An exception to this is the falciform
ligament, which attaches the liver to the posterior portion of the anterior body
wall.
Lobes
Traditional
gross
anatomy divided the liver into two lobes (left and right), if viewed from
the parietal surface; but if observed on the visceral surface it is divided into
four lobes with the addition of the caudate and quadrate lobe.
The
falciform ligament is visible on the front (anterior
side) of the liver. This divides the liver into a
left anatomical lobe, and a
right anatomical lobe.
If the liver is flipped over, to look at it from below (the
visceral surface), there are two additional lobes between the right and
left. These are the
caudate lobe (the more superior) and the
quadrate lobe (the more inferior).
On the visceral surface a functional anatomy dictates how the liver is
organized. One must view an imaginary line that passes to the left of the vena
cava all the way forward and sections the gallblader into two halfs. This line
is called Cantlie's Line. This line divides the liver in left and right. Other
anatomical landmarks exist, such as the ligamentum venosum (ligamentum of
Arancio) and the round ligament (ligamentum Teres) that further divide the left
side of the liver in two sections. Now an important anatomical landmark, the
transverse fissure of the liver divides this left portion of the liver into four
segments which will be numbered starting at the caudate lobule as I in an
anti-clock manner. From this visceral view we can see 7 segments because the 8th
segment is only visible in the parietal view. Each of the lobes is made up of
lobules; a vein goes from the centre, which then joins to the hepatic vein to
carry blood out from the liver.
On the surface of the lobules, there are ducts, veins and arteries that carry
fluids to and from them.
Functional anatomy
Correspondence between anatomic lobes and Couinaud segments
| Segment* |
Couinaud segments |
| Caudate |
1 |
| Lateral |
2, 3 |
| Medial |
4a, 4b |
| Right |
5, 6, 7, 8 |
|
* or lobe, in the case of the caudate lobe
Each number in the list corresponds to one in the table. 1. Caudate
2. Superior subsegment of the lateral segment
3. Inferior subsegment of the lateral segment
4a. Superior subsegment of the medial segment
4b. Inferior subsegment of the medial segment
5. Inferior subsegment of the anterior segment
6. Inferior subsegment of the posterior segment
7. Superior subsegment of the posterior segment
8. Superior subsegment of the anterior segment
|
The central area where the
common bile duct,
hepatic portal vein, and
hepatic artery proper enter is the
hilum or "porta
hepatis". The duct, vein, and artery divide into left and right branches,
and the portions of the liver supplied by these branches constitute the
functional left and right lobes.
The functional lobes are separated by an imaginary plane (historically called
Cantlie's line) joining the gallbladder fossa to the inferior vena cava.
The plane separates the liver into the true right and left lobes. The middle
hepatic vein also demarcates the true right and left lobes. The right lobe is
further divided into an
anterior and
posterior segment by the right hepatic vein. The left lobe is divided into
the medial and
lateral segments by the left hepatic vein. The fissure for the
ligamentum teres also separates the medial and lateral segments. The medial
segment is also called the
quadrate lobe. In the widely used
Couinaud (or "French") system, the functional lobes are further divided into
a total of eight subsegments based on a transverse plane through the bifurcation
of the main portal vein. The
caudate lobe is a separate structure which receives blood flow from both the
right- and left-sided vascular branches.[7][8]
In other animals
The liver is found in all
vertebrates,
and is typically the largest
visceral organ. Its form varies considerably in different species, and is
largely determined by the shape and arrangement of the surrounding organs.
Nonetheless, in most species it is divided into right and left lobes; exceptions
to this general rule include
snakes, where the
shape of the body necessitates a simple cigar-like form. The internal structure
of the liver is broadly similar in all vertebrates.[9]
An organ sometimes referred to as a liver is found associated with the
digestive tract of the primitive chordate
Amphioxus. However, this is an enzyme secreting gland, not a metabolic
organ, and it is unclear how truly
homologous it is to the vertebrate liver.[9]
Physiology
The various functions of the liver are carried out by the liver cells or
hepatocytes.
Currently, there is no
artificial organ or device capable of emulating all the functions of the
liver. Some functions can be emulated by
liver dialysis, an experimental treatment for
liver
failure. The liver is thought to be responsible for up to 500 separate
functions, usually in combination with other systems and organs.
Synthesis

A CT scan in which the liver and portal vein are shown.
- A large part of
amino acid synthesis
- The liver performs several roles in
carbohydrate metabolism:
- The liver is responsible for the mainstay of protein
metabolism, synthesis as well as degradation.
- The liver also performs several roles in
lipid
metabolism:
- The liver produces
coagulation factors
I
(fibrinogen),
II
(prothrombin),
V,
VII,
IX,
X and
XI,
as well as
protein C,
protein S
and
antithrombin.
- In the first trimester
fetus, the
liver is the main site of
red blood cell production. By the 32nd week of
gestation,
the
bone marrow has almost completely taken over that task.
- The liver produces and excretes
bile (a
yellowish liquid) required for emulsifying fats and help the absorption of
vitamin K from the diet. Some of the bile drains directly into the
duodenum,
and some is stored in the
gallbladder.
- The liver also produces
insulin-like growth factor 1 (IGF-1), a
polypeptide
protein
hormone that plays an important role in childhood growth and continues to
have
anabolic effects in adults.
- The liver is a major site of
thrombopoietin production. Thrombopoietin is a
glycoprotein hormone that regulates the production of
platelets
by the
bone
marrow.
Breakdown
Other functions
- The liver stores a multitude of substances, including glucose (in the
form of
glycogen),
vitamin A
(1–2 years' supply),
vitamin D
(1–4 months' supply)[citation
needed],
vitamin B12 (1–3 years' supply),
vitamin K,
iron, and
copper.
- The liver is responsible for immunological effects—the
reticuloendothelial system of the liver contains many immunologically
active cells, acting as a 'sieve' for antigens carried to it via the
portal system.
- The liver produces
albumin,
the major
osmolar component of
blood serum.
- The liver synthesizes
angiotensinogen, a hormone that is responsible for raising the
blood pressure when activated by
renin, an
enzyme that is released when the
kidney senses
low
blood pressure.
Relation to medicine and pharmacology
The oxidative capacity of the liver decreases with aging and therefore,
benzodiazepines (BZDs) that require oxidation are more likely to accumulate
to toxic levels. Therefore, those with shorter half-lives, such as
lorazepam
and oxazepam
are preferred when benzodiazepines are required in regards to
geriatric medicine.
Diseases of the liver
Main article:
Liver diseaseThe liver supports almost every organ in the body and is vital for survival.
Because of its strategic location and multidimensional functions, the liver is
also prone to many diseases.[10]
The most common include: Infections such as
hepatitis A, B, C, D, E,
alcohol damage,
fatty
liver,
cirrhosis,
cancer, drug damage (particularly by
acetaminophen (paracetamol) and cancer drugs).
Many diseases of the liver are accompanied by
jaundice
caused by increased levels of
bilirubin
in the system. The bilirubin results from the breakup of the
hemoglobin of dead
red
blood cells; normally, the liver removes bilirubin from the blood and
excretes it through bile.
There are also many pediatric liver diseases including
biliary atresia,
alpha-1 antitrypsin deficiency,
alagille syndrome,
progressive familial intrahepatic cholestasis, and
Langerhans cell histiocytosis, to name but a few.
Diseases that interfere with liver function will lead to derangement of these
processes. However, the liver has a great capacity to
regenerate and has a large reserve capacity. In most cases, the liver only
produces symptoms after extensive damage.
Liver diseases may be diagnosed by
liver function tests, for example, by production of
acute phase proteins.
Disease symptoms
The classic symptoms of liver damage include the following:
- Pale stools occur when
stercobilin, a brown pigment, is absent from the stool. Stercobilin is
derived from bilirubin metabolites produced in the liver.
- Dark urine occurs when bilirubin mixes with urine
- Jaundice (yellow skin and/or whites of the eyes) This is where
bilirubin
deposits in skin, causing an intense
itch. Itching
is the most common complaint by people who have liver failure. Often this
itch cannot be relieved by drugs.
-
Swelling of the abdomen, ankles and feet occurs because the liver
fails to make
albumin.
- Excessive fatigue occurs from a generalized loss of nutrients,
minerals and vitamins.
- Bruising
and easy bleeding are other features of liver disease. The liver makes
substances which help prevent bleeding. When liver damage occurs, these
substances are no longer present and severe bleeding can occur.[11]
Diagnosis
The diagnosis of liver function is made by
blood tests.
Liver function tests can readily pinpoint the extent of liver damage. If
infection
is suspected, then other
serological
tests are done. Sometimes, one may require an
ultrasound
or a
CT scan to produce an image of the liver.
Physical examination of the liver is not accurate in determining the extent
of liver damage. It can only reveal presence of tenderness or the size of liver,
but in all cases, some type of radiological study is required to examine it.[12]
Biopsy / scan
Damage to the liver is sometimes determined with a
biopsy,
particularly when the cause of liver damage is unknown. In the 21st century they
were largely replaced by high-resolution radiographic scans. The latter do not
require ultrasound guidance, lab involvement, microscopic analysis, organ
damage, pain, or patient sedation; and the results are available immediately on
a computer screen.
In a biopsy, a needle is inserted into the skin just below the rib cage and a
tissue sample obtained. The tissue is sent to the laboratory, where it is
analyzed under a
microscope.
Sometimes, a radiologist may assist the physician performing a
liver
biopsy by providing ultrasound guidance.[13]
Regeneration
The liver is the only human internal organ capable of natural
regeneration of lost
tissue; as little as 25% of a liver can regenerate into a whole liver.[14]
This is, however, not true regeneration but rather
compensatory growth.[15]
The lobes that are removed do not regrow and the growth of the liver is a
restoration of function, not original form. This contrasts with true
regeneration where both original function and form are restored. In liver, large
areas of the tissues are formed but for the formation of new cells there must be
sufficient amount of material so the circulation of the blood becomes more
active.
[16]
This is predominantly due to the
hepatocytes
re-entering the
cell cycle.
That is, the hepatocytes go from the quiescent
G0 phase to
the G1 phase
and undergo mitosis. This process is activated by the
p75
receptors.[17]
There is also some evidence of
bipotential
stem cells,
called hepatic oval cells or ovalocytes (not to be confused with oval red blood
cells of
ovalocytosis), which are thought to reside in the
canals of Hering. These cells can differentiate into either
hepatocytes
or
cholangiocytes, the latter being the cells that line the
bile ducts.
Scientific and medical works about liver regeneration often refer to the
Greek
Titan
Prometheus who was chained to a rock in the Caucasus where, each day, his
liver was devoured by an eagle, only to grow back each night. The myth suggests
the
ancient Greeks knew about the liver’s remarkable capacity for self-repair,
however, this claim is without evidence.[18]
Liver transplantation
Human liver transplants were first performed by
Thomas Starzl in the
United States and
Roy Calne in
Cambridge,
England in
1963 and 1965, respectively.
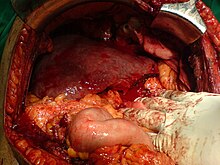
After resection of left lobe liver tumor
Liver transplantation is the only option for those with irreversible liver
failure. Most transplants are done for chronic liver diseases leading to
cirrhosis,
such as chronic
hepatitis
C,
alcoholism, autoimmune hepatitis, and many others. Less commonly, liver
transplantation is done for
fulminant hepatic failure, in which liver failure occurs over days to weeks.
Liver
allografts for
transplant usually come from donors who have died from fatal
brain injury.
Living donor liver transplantation is a technique in which a portion of a
living person's liver is removed and used to replace the entire liver of the
recipient. This was first performed in 1989 for pediatric liver transplantation.
Only 20 percent of an adult's liver (Couinaud segments 2 and 3) is needed to
serve as a liver allograft for an infant or small child.
More recently, adult-to-adult liver transplantation has been done using the
donor's right hepatic lobe, which amounts to 60 percent of the liver. Due to the
ability of the liver to
regenerate, both the donor and recipient end up with normal liver function
if all goes well. This procedure is more controversial, as it entails performing
a much larger operation on the donor, and indeed there have been at least two
donor deaths out of the first several hundred cases. A recent publication has
addressed the problem of donor mortality, and at least 14 cases have been found.[19]
The risk of postoperative complications (and death) is far greater in
right-sided operations than that in left-sided operations.
With the recent advances of noninvasive imaging, living liver donors usually
have to undergo imaging examinations for liver anatomy to decide if the anatomy
is feasible for donation. The evaluation is usually performed by multidetector
row
computed tomography (MDCT) and
magnetic resonance imaging (MRI). MDCT is good in vascular anatomy and
volumetry. MRI is used for biliary tree anatomy. Donors with very unusual
vascular anatomy, which makes them unsuitable for donation, could be screened
out to avoid unnecessary operations.
-
MDCT image. Arterial anatomy contraindicated for liver donation
-
MDCT image. Portal venous anatomy contraindicated for liver donation
-
MDCT image. 3D image created by MDCT can clearly visualize the
liver, measure the liver volume, and plan the dissection plane to
facilitate the liver transplantation procedure.
-
Phase contrast CT image. Contrast is perfusing the right liver but
not the left due to a left portal vein thrombus.
Development
Organogenesis
The origins of the liver lie in both the ventral portion of the
foregut
endoderm
(endoderm being one of the 3 embryonic germ cell layers) and the constituents of
the adjacent
septum transversum
mesenchyme.
In human embryo,
the
hepatic diverticulum is the tube of endoderm that extends out from the
foregut into the surrounding mesenchyme. The mesenchyme of septum transversum
induces this endoderm to proliferate, to branch, and to form the glandular
epithelium of the liver. A portion of the hepatic diverticulum (that region
closest to the digestive tube) continues to function as the
drainage duct of the liver, and a branch from this duct produces the
gallbladder.[20]
Besides of signals from the septum transversum mesenchyme,
fibroblast growth factor from the
developing heart also contribute to hepatic competence, along with
retinoic acid emanating from the
lateral plate mesoderm. The hepatic endodermal cells undergo a morphological
transition from columnar to pseudostratified resulting in thickening into the
early
liver bud. Their expansion forms a population of the bipotential
hepatoblasts.[21]
Hepatic stellate cells are derived from mesenchyme.[22]
After migration of hepatoblasts into the septum transversum mesenchyme, the
hepatic architecture begins to be established, with
liver sinusoids and bile canaliculi appearing. The liver bud separates into
the lobes. The left
umbilical vein becomes the
ductus venosus and the right
vitelline vein becomes the
portal vein. The expanding liver bud is colonized by
hematopoietic cells. The bipotential hepatoblasts begin differentiating into
biliary epithelial cells and
hepatocytes.
The biliary epithelial cells differentiate from hepatoblasts around portal
veins, first producing a monolayer, and then a bilayer of cuboidal cells. In
ductal plate, focal dilations emerge at points in the bilayer, become surrounded
by portal mesenchyme, and undergo tubulogenesis into intrahepatic bile ducts.
Hepatoblasts not adjacent to portal veins instead differentiate into hepatocytes
and arrange into cords lined by sinudoidal epithelial cells and bile canaliculi.
Once hepatoblasts are specified into hepatocytes and undergo further expansion,
they begin acquiring the functions of a mature hepatocyte, and eventually mature
hepatocytes appear as highly polarized epithelial cells with abundant
glycogen
accumulation. In the adult liver, hepatocytes are not equivalent, with position
along the portocentrovenular axis within a
liver lobule dictating expression of metabolic genes involved in drug
metabolism, carbohydrate metabolism, ammonia detoxification, and bile production
and secretion.
WNT/β-catenin has now been identified to be playing a key role in this
phenomenon.[21]
Fetal blood supply
In the growing fetus, a major source of blood to the liver is the
umbilical vein which supplies nutrients to the growing fetus. The umbilical
vein enters the abdomen at the umbilicus, and passes upward along the free
margin of the
falciform ligament of the liver to the inferior surface of the liver. There
it joins with the left branch of the portal vein. The
ductus venosus carries blood from the left portal vein to the left hepatic
vein and then to the
inferior vena cava, allowing placental blood to bypass the liver.
In the fetus, the liver develops throughout normal gestation, and does not
perform the normal filtration of the infant liver. The liver does not perform
digestive processes because the fetus does not consume meals directly, but
receives nourishment from the mother via the
placenta.
The fetal liver releases some blood stem cells that migrate to the fetal
thymus, so
initially the
lymphocytes, called
T-cells, are created from fetal liver stem cells. Once the fetus is
delivered, the formation of blood stem cells in infants shifts to the red
bone
marrow.
After birth, the umbilical vein and ductus venosus are completely obliterated
in two to five days; the former becomes the
ligamentum teres and the latter becomes the
ligamentum venosum. In the disease state of
cirrhosis
and
portal hypertension, the umbilical vein can open up again.
As food
Main article:
Liver (food)The liver of mammals,
fowl, and fish are
commonly eaten as food
by humans.
Domestic pig, ox,
lamb, calf,
chicken, and
goose livers are
widely available from butchers and supermarkets.
Liver can be baked, boiled, broiled, fried,
stir-fried, or eaten raw (asbeh nayeh or sawda naye in
Lebanese cuisine, liver
sashimi). In
many preparations, pieces of liver are combined with pieces of meat or kidneys,
like in the various forms of Middle Eastern
mixed
grill (e.g.
meurav Yerushalmi). Liver is often made into
spreads. Well-known examples include
liver pâté,
foie gras,
chopped liver, and
leverpastej. Liver
sausages such
as
Braunschweiger and
liverwurst
are also a valued meal.
Liver sausages may also be used as spreads. A traditional
South African delicacy, namely
Skilpadjies, is made of minced lamb's liver wrapped in netvet (caul
fat), and grilled over an open fire.
Animal livers are rich in iron and
vitamin A,
and
cod liver oil is commonly used as a
dietary supplement. Traditionally, some fish livers were valued as food,
especially the
stingray liver. It was used to prepare delicacies, such as poached skate
liver on toast in England, as well as the beignets de foie de raie and
foie de raie en croute in
French cuisine.[23]
Cultural allusions
In
Greek mythology,
Prometheus
was punished by the gods for revealing fire to humans, by being chained to a
rock where a
vulture (or an
eagle) would peck out his liver, which would regenerate overnight. (The
liver is the only human internal organ that actually can regenerate itself to a
significant extent.) Many ancient peoples of the Near East and Mediterranean
areas practiced a type of
divination
called
haruspicy, where they tried to obtain information by examining the livers of
sheep and other animals.
In Plato, and in later physiology, the liver was thought to be the seat of
the darkest emotions (specifically wrath, jealousy and greed) which drive men to
action.[24]
The Talmud
(tractate Berakhot 61b) refers to the liver as the seat of
anger, with the
gallbladder counteracting this.
The
Persian, Urdu,
and Hindi
languages (جگر or जिगर or jigar) refer to the liver in figurative speech
to indicate courage and strong feelings, or "their best"; e.g., "This
Mecca has thrown
to you the pieces of its liver!".[25]
The term jan e jigar, literally "the strength (power) of my liver", is a
term of endearment in Urdu. In Persian slang, jigar is used as an
adjective for any object which is desirable, especially women. In the
Zulu
language, the word for liver (isibindi) is the same as the word for courage.
The legend of
Liver-Eating Johnson says that he would cut out and eat the liver of each
man killed after dinner.
In the motion picture
The Message,
Hind bint Utbah is implied or portrayed eating the liver of
Hamza ibn ‘Abd al-Muttalib during the
Battle of Uhud. Although there are narrations that suggest that Hind did
"taste", rather than eat, the liver of Hamza, the authenticity of these
narrations have to be questioned.
Additional Images
-
-
-
-
Dissection of portal vein in right lobe of liver]]
-
Human embryo, 38 mm, 8–9 weeks.
See also
