-
Disease
-
Arthritis
-
Kidney
-
Organ donation
-
Euthanasia
-
Pregnancy
-
Hand
-
Fine motor skill
-
Drug rehabilitation
-
Cataract
-
Aging-associated diseases
-
Nursing home
-
Support group
-
Psychiatry
-
Lobotomy
-
Sneeze
-
Virus
-
Ambulance
-
Dialysis
-
Medical imaging
-
Medical test
-
Complete blood count
-
Hospital-acquired infection
-
Pneumonia
-
Elsevier
-
Pharmaceutical industry
-
Generic drug
-
Antibiotic resistance
-
Bioavailability
-
Dietary supplement
-
HIV / AIDS
-
Epidemic
-
Ignaz Semmelweis
-
Wart
-
Heat illness
-
Heart rate
-
Blood group systems
-
International Society of Blood Transfusion
-
Cardiopulmonary resuscitation
-
Unified Medical Language System
-
Self-diagnosis
-
Homeopathy
-
Naturopathy
-
Massage
-
Drowning
-
Nose
-
Influenza
-
Anorexia (symptom)
-
Weight loss
-
Exercise physiology
|
Pregnancy

Text is available under the
Creative Commons Attribution-ShareAlike License; additional
terms may apply. See
Terms of
Use for details.
Wikipedia® is a registered trademark of the
Wikimedia Foundation,
Inc., a non-profit organization.
Traduzione
interattiva on/off
- Togli il segno di spunta per disattivarla

Pregnancy is the
fertilization and development of one or more offspring,
known as an
embryo or
fetus,
in a woman's
uterus. In a pregnancy, there can be multiple
gestations, as in the case of twins or
triplets.
Childbirth usually occurs about 38 weeks after conception;
in women who have a menstrual cycle length of four weeks, this
is approximately 40 weeks from the start of the last normal
menstrual period (LNMP). Human pregnancy is the most studied of
all
mammalian pregnancies. Conception can be achieved through
sexual intercourse or
assisted reproductive technology. An
embryo is the developing offspring during the first 8
weeks following conception, and subsequently the term fetus
is used until birth.[1][2]
In many societies' medical or legal definitions, human pregnancy
is somewhat arbitrarily divided into three trimester periods, as
a means to simplify reference to the different stages of
prenatal development. The first trimester carries the
highest risk of
miscarriage (natural death of embryo or fetus). During the
second trimester, the development of the fetus can be more
easily monitored and diagnosed. The beginning of the third
trimester often approximates the point of
viability, or the ability of the fetus to survive, with or
without medical help, outside of the
uterus.[3]
In the United States and United Kingdom, 40% of pregnancies
are
unplanned, and between a quarter and half of those unplanned
pregnancies were
unwanted pregnancies.[4][5]
Of those unintended pregnancies that occurred in the US, 60% of
the women used
birth control to some extent during the month pregnancy
occurred.[6]
Terminology
One scientific term for the state of pregnancy is
gravidity (adjective "gravid"),
Latin
for "heavy" and a pregnant female is sometimes referred to as a
gravida.[7]
Similarly, the term
parity (abbreviated as "para") is used for the number of
times a female has given birth, counting twins and other
multiple births as one pregnancy, and usually including
stillbirths. Medically, a woman who has never been pregnant
is referred to as a nulligravida, a woman who is (or has
been only) pregnant for the first time as a primigravida,[8]
and a woman in subsequent pregnancies as a
multigravida or multiparous.[7][9]
Hence, during a second pregnancy a woman would be described as
gravida 2, para 1 and upon live delivery as gravida 2,
para 2. An in-progress pregnancy, as well as
abortions,
miscarriages, or
stillbirths account for parity values being less than the
gravida number. In the case of twins, triplets etc., gravida
number and parity value are increased by one only. Women who
have never carried a pregnancy achieving more than 20 weeks of
gestation age are referred to as nulliparous.[10]
Progression
Initiation

Fertilization and implantation in humans.
Although pregnancy begins with
implantation, the process leading to pregnancy occurs
earlier as the result of the female
gamete, or
oocyte, merging with the male gamete,
spermatozoon. In medicine, this process is referred to as
fertilization; in lay terms, it is more commonly known as
"conception." After the point of
fertilization, the fused product of the female and male
gamete is referred to as a
zygote or fertilized egg. The fusion of male and female
gametes usually occurs following the act of
sexual intercourse, resulting in spontaneous pregnancy.
However, the advent of
assisted reproductive technology such as
artificial insemination and
in vitro fertilisation have made achieving pregnancy
possible without engaging in sexual intercourse. This approach
may be undertaken as a voluntary choice or due to
infertility.
The process of fertilization occurs in several steps, and the
interruption of any of them can lead to failure. Through
fertilization, the
egg is activated to begin its developmental process, and the
haploid
nuclei of the two gametes come together to form the
genome of a new
diploid
organism.
At the beginning of the process, the sperm undergoes a series
of changes, as freshly ejaculated sperm is unable or poorly able
to fertilize.[11]
The sperm must undergo
capacitation in the female's reproductive tract over several
hours, which increases its motility and destabilizes its
membrane, preparing it for the
acrosome reaction, the enzymatic penetration of the egg's
tough membrane, the
zona pellucida, which surrounds the oocyte. The sperm and
the egg cell, which has been released from one of the female's
two
ovaries, unite in one of the two
fallopian tubes. The fertilized egg, known as a
zygote, then moves toward the uterus, a journey that can
take up to a week to complete. Cell division begins
approximately 24 to 36 hours after the male and female cells
unite. Cell division continues at a rapid rate and the cells
then develop into what is known as a
blastocyst. The blastocyst is made up of three layers: the
ectoderm (which will become the skin and nervous system), the
endoderm (which will become the digestive and respiratory
systems), and the mesoderm (which will become the muscle and
skeletal systems). Finally, the blastocyst arrives at the uterus
and attaches to the uterine wall, a process known as
implantation.
The mass of cells, now known as an embryo, begins the
embryonic stage, which continues until cell differentiation is
almost complete at eight weeks. Structures important to the
support of the embryo develop, including the
placenta and
umbilical cord. During this time, cells begin to
differentiate into the various body systems. The basic outlines
of the organ, body, and nervous systems are established. By the
end of the embryonic stage, the beginnings of features such as
fingers, eyes, mouth, and ears become visible.
Once cell differentiation is mostly complete, the embryo
enters the final stage and becomes known as a fetus. The early
body systems and structures that were established in the
embryonic stage continue to develop. Sex organs begin to appear
during the third month of gestation. The fetus continues to grow
in both weight and length, although the majority of the physical
growth occurs in the last weeks of pregnancy.
Duration
Healthcare professionals name three different dates as the
start of pregnancy:
- the first day of the woman's last normal
menstrual period, and the resulting fetal age is called
the
gestational age
- the date of conception (about two weeks before her
next expected menstrual period), with the age called
fertilization age
- the date of implantation (about one week after
conception).
Since these are spread over a significant period of time, the
duration of pregnancy necessarily depends on the date selected
as the starting point chosen.
As measured on a
reference group of women with a
menstrual cycle of exactly 28-days prior to pregnancy, and
who had spontaneous onset of labor, the mean pregnancy length
has been estimated to be 283.4 days of
gestational age as timed from the first day of the
last menstrual period as recalled by the mother, and 280.6
days when the gestational age was retrospectively estimated by
obstetric ultrasound measurement of the
fetal biparietal diameter (BPD) in the second trimester.[12]
Other algorithms take into account a variety of other variables,
such as whether this is the first or subsequent child (i.e.,
pregnant woman is a primipara or a
multipara, respectively), the mother's race, parental age,
length of menstrual cycle, and menstrual regularity), but these
are rarely used by healthcare professionals. In order to have a
standard reference point, the normal pregnancy duration is
generally assumed to be 280 days (or 40 weeks) of gestational
age.
There is a
standard deviation of 8–9 days surrounding due dates
calculated with even the most accurate methods. This means that
fewer than 5 percent of births occur on the day of being 40
weeks of gestational age; 50 percent of births are within a week
of this duration, and about 80 percent are within 2 weeks.[12]
It is much more useful and accurate, therefore, to consider a
range of due dates, rather than one specific day, with some
online due date calculators providing this information.[13]
The most common system used among healthcare professionals is
Naegele's rule, which was developed in the early 19th
century. This calculates the expected due date from the first
day of the last normal menstrual period (LMP or LNMP) regardless
of factors known to make this inaccurate, such as a shorter or
longer menstrual cycle length. Pregnancy most commonly lasts for
40 weeks according to this LNMP-based method, assuming that the
woman has a predictable menstrual cycle length of close to 28
days and conceives on the 14th day of that cycle
Accurate dating of pregnancy is important, because it is used
in calculating the results of various
prenatal tests, (for example, in the
triple test). A decision may be made to
induce labour if a fetus is perceived to be overdue.
Furthermore, if LMP and ultrasound dating predict different
respective due dates, with the latter being later, this might
signify slowed fetal growth and therefore require closer review.
The age of
fetal viability has been receding because of continued
medical progress. Whereas it used to be 28 weeks, it has been
brought back to as early as 23, or even 22 weeks in some
countries.[citation
needed]
Preterm, term and postterm
Pregnancy is considered "at term" when
gestation has lasted 37 complete weeks (occurring at the
transition from the 37th to the 38th week of gestation), but is
less than 42 weeks of gestational age (occurring at the
transition from the 42nd week to the 43rd week of gestation, or
between 259 and 294 days since LMP). "Full term" refers
to the gestation having lasted 40
weeks
from the first day of the mother's last
menstrual period. This is the end of gestation on average.
Alternatively expressed, this corresponds to a
gestational age of 40 weeks and 0 days, or 280 days, or
approximately 9 months, and occurs at the transition from the
40th to the 41st week of gestation. On average, it corresponds
to an
embryonic age of 38 weeks or 266 days.
Events before completion of 37 weeks (259 days) are
considered
preterm; from week 42 (294 days) events are considered
postterm.[14]
When a pregnancy exceeds 42 weeks (294 days), the risk of
complications for both the woman and the fetus increases
significantly.[15][16]
Therefore, in an otherwise uncomplicated pregnancy,
obstetricians usually prefer to
induce labour at some stage between 41 and 42 weeks.[17][18]
Birth before 39 weeks by C section, even if considered "at
term", results in an increases risk of complications and
premature death, when not medically needed.[19]
This is from factors including underdeveloped lungs, infection
due to underdeveloped immune system, problems feeding due to
underdeveloped brain, and
jaundice from underdeveloped liver. Some hospitals in the
United States have noted a significant increase in
neonatal intensive care unit patients when women schedule
deliveries for convenience and are taking steps to reduce
induction for non-medical reasons.[20]
Complications from
Caesarean section are more common than for live births.
Recent medical literature prefers the terminology preterm
and postterm to premature and postmature.
Preterm and postterm are unambiguously defined as
above, whereas premature and postmature have
historical meaning and relate more to the infant's size and
state of development rather than to the stage of pregnancy.[21][22]
Childbirth
Childbirth is the process whereby an infant is born.
A woman is considered to be in labour when she begins
experiencing regular uterine contractions, accompanied by
changes of her cervix – primarily effacement and dilation. While
childbirth is widely experienced as painful, some women do
report painless labours, while others find that concentrating on
the birth helps to quicken labour and lessen the sensations.
Most births are successful vaginal births, but sometimes
complications arise and a woman may undergo a
cesarean section.
During the time immediately after birth, both the mother and
the baby are hormonally cued to bond, the mother through the
release of
oxytocin, a hormone also released during
breastfeeding. Studies show that skin-to-skin contact
between a mother and her newborn immediately after birth is
beneficial for both the mother and baby. A review done by the
World Health Organization found that skin-to-skin contact
between mothers and babies after birth reduces crying, improves
mother-infant interaction, and helps mothers to breastfeed
successfully. They recommend that
neonates be allowed to bond with the mother during their
first two hours after birth, the period that they tend to be
more alert than in the following hours of early life.[23]
Postnatal
period
The postnatal period begins immediately after the birth of a
child and then extends for about six weeks. During this period,
the mother's body begins the return to prepregnancy conditions
that includes changes in hormone levels and uterus size.
Diagnosis
The beginning of pregnancy may be detected either based on
symptoms by the pregnant woman herself, or by using medical
tests with or without the assistance of a medical professional.
Approximately 1 in 475 women at 20 weeks, and 1 in 2500 women at
delivery, refuse to acknowledge that they are pregnant, which is
called
denial of pregnancy.[24]
Some non-pregnant women have a very strong belief that they are
pregnant along with some of the physical changes. This condition
is known as
pseudocyesis or false pregnancy.[25]
Physical signs
Most pregnant women experience a number of symptoms,[26]
which can signify pregnancy. The symptoms can include nausea and
vomiting, excessive tiredness and fatigue,
cravings for certain foods that are not normally sought out,
and frequent urination particularly during the night.
A number of early
medical signs are associated with pregnancy.[27][28]
These signs typically appear, if at all, within the first few
weeks after conception. Although not all of these signs are
universally present, nor are all of them diagnostic by
themselves, taken together they make a presumptive diagnosis of
pregnancy. These signs include the presence of
human chorionic gonadotropin (hCG) in the blood and urine,
missed
menstrual period, implantation bleeding that occurs at
implantation of the embryo in the uterus during the third or
fourth week after last menstrual period, increased
basal body temperature sustained for over 2 weeks after
ovulation,
Chadwick's sign (darkening of the
cervix,
vagina, and
vulva),
Goodell's sign (softening of the vaginal portion of the
cervix),
Hegar's sign (softening of the
uterus
isthmus), and pigmentation of linea alba –
Linea nigra, (darkening of the skin in a midline of the
abdomen, caused by
hyperpigmentation resulting from hormonal changes, usually
appearing around the middle of pregnancy).[27][28]
Breast tenderness is common during the first trimester, and
is more common in women who are pregnant at a young age.[29]
Despite all the signs, some women may not realize they are
pregnant until they are far along in pregnancy. In some cases, a
few have not been aware of their pregnancy until they begin
labour. This can be caused by many factors, including
irregular periods (quite common in teenagers), certain
medications (not related to conceiving children), and
obese women who disregard their weight gain. Others may be
in
denial of their situation.
Tests
Pregnancy detection can be accomplished using one or more
various
pregnancy tests,[30]
which detect hormones generated by the newly formed
placenta. Blood and urine tests can detect pregnancy 12 days
after implantation.[31]
Blood pregnancy tests are more sensitive than urine tests
(giving fewer false negatives).[32]
Home
pregnancy tests are
urine
tests, and normally detect a pregnancy 12 to 15 days after
fertilization. A quantitative blood test can determine
approximately the date the embryo was conceived. Testing 48
hours apart can provide useful information regarding how the
pregnancy is doing. A single test of
progesterone levels can also help determine how likely a
fetus will survive in those with a
threatened miscarriage (bleeding in early pregnancy).[33]
An early
obstetric ultrasonography can determine the age of the
pregnancy fairly accurately. In practice, medical professionals
typically express the age of a pregnancy (i.e., an "age" for an
embryo) in terms of "menstrual date" based on the first day
of a woman's last menstrual period, as the woman reports it.
Unless a woman's recent
sexual activity has been limited, she has been charting her
cycles, or the conception is the result of some types of
fertility treatment (such as
IUI or
IVF), the exact date of fertilization is unknown. Without
symptoms such as
morning sickness, often the only visible sign of a pregnancy
is an interruption of the woman's normal monthly menstruation
cycle, (i.e., a "late period"). Hence, the "menstrual date" is
simply a common educated estimate for the age of a fetus, which
is an average of 2 weeks later than the first day of the woman's
last menstrual period. The term "conception date" may sometimes
be used when that date is more certain, though even medical
professionals can be imprecise with their use of the two
distinct terms. The due date can be calculated by using
Naegele's rule. The expected date of delivery may also be
calculated from
sonogram measurement of the fetus. This method is slightly
more accurate than methods based on LMP.[34]
Additional
obstetric diagnostic techniques can estimate the health and
presence or absence of
congenital diseases at an early stage.
Ultrasound
One way to observe prenatal development is via ultrasound
images. Ultrasound imaging before 24 weeks can help determine
the due date and detect multiple pregnancies[35]
however in those who are at low risk it is unclear if this makes
a significant difference in outcomes.[36]
Routine ultrasound imaging after 24 weeks gestation does not
improve outcomes in either the mother or the baby and might
increase the risk of a cesarean section.[37]
It is thus is not recommended.[36]
Modern
3D ultrasound images provide greater detail for prenatal
diagnosis than the older 2D ultrasound technology.[38]
While 3D is popular with parents desiring a prenatal photograph
as a keepsake,[39]
both 2D and 3D are discouraged by the
FDA for non-medical use,[40]
but there are no definitive studies linking ultrasound to any
adverse medical effects.[41]
The following 3D ultrasound images were taken at different
stages of pregnancy:
-
3D Ultrasound of fetal movements at 12 weeks
-
-
-
Physiology

Breast changes as seen during pregnancy. Note the
increase in size and darkening of the areola.
Pregnancy is typically broken into three periods, or
trimesters, each of about three months.[42][43]
Obstetricians define each trimester as lasting for 14 weeks,
resulting in a total duration of 42 weeks, although the average
duration of pregnancy is actually about 40 weeks.[44]
While there are no hard and fast rules, these distinctions are
useful in describing the changes that take place over time.
First
trimester
Traditionally, medical professionals have measured pregnancy
from a number of convenient points, including the day of last
menstruation, ovulation, fertilization, implantation and
chemical detection. In medicine, pregnancy is often defined as
beginning when the developing
embryo becomes
implanted in the
endometrial lining of a woman's
uterus. Most pregnant women do not have any specific signs
or symptoms of implantation, although it is not uncommon to
experience minimal bleeding. After implantation, the uterine
endometrium is called the
decidua. The
placenta, which is formed partly from the decidua and partly
from outer layers of the embryo, connects the developing embryo
to the uterine wall to allow nutrient uptake, waste elimination,
and gas exchange via the mother's blood supply. The
umbilical cord is the connecting cord from the embryo or
fetus to the placenta. The developing embryo undergoes
tremendous growth and changes during the process of
fetal development.
Morning sickness occurs in about seventy percent of all
pregnant women, and typically improves after the first
trimester.[45]
Although described as "morning sickness", women can experience
this nausea during afternoon, evening, and throughout the entire
day.
Shortly after conception, the nipples and areolas begin to
darken due to a temporary increase in hormones.[46]
This process continues throughout the pregnancy.
The first 12 weeks of pregnancy are considered to make up the
first trimester. The first two weeks from the first trimester
are calculated as the first two weeks of pregnancy even though
the pregnancy does not actually exist. These two weeks are the
two weeks before conception and include the woman's last
period.
The third week is the week in which fertilization occurs and
the 4th week is the period when
implantation takes place. In the 4th week, the fecundated
egg reaches the
uterus and burrows into its wall which provides it with the
nutrients it needs. At this point, the zygote becomes a
blastocyst and the
placenta starts to form. Moreover, most of the pregnancy
tests may detect a pregnancy beginning with this week.
The 5th week marks the start of the
embryonic period. This is when the embryo's
brain,
spinal cord,
heart and other organs begin to form.[47]
At this point the embryo is made up of three layers, of which
the top one (called the
ectoderm) will give rise to the embryo's outermost layer of
skin, central and peripheral
nervous systems,
eyes,
inner ear, and many
connective tissues.[47]
The heart and the beginning of the
circulatory system as well as the
bones,
muscles and
kidneys are made up from the
mesoderm (the middle layer). The inner layer of the embryo
will serve as the starting point for the development of the
lungs,
intestine and
bladder. This layer is referred to as the
endoderm. An embryo at 5 weeks is normally between
1⁄16
and 1⁄8
inch (1.6 and 3.2 mm) in length.
In the 6th week, the embryo will be developing basic facial
features and its arms and legs start to grow. At this point, the
embryo is usually no longer than
1⁄6
to 1⁄4
inch (4.2 to 6.4 mm). In the following week, the brain, face and
arms and legs quickly develop. In the 8th week, the embryo
starts moving and in the next 3 weeks, the embryo's toes,
neck
and
genitals develop as well. According to the American
Pregnancy Association, by the end of the first trimester, the
fetus
will be about 3 inches (76 mm) long and will weigh approximately
1 ounce (28 g).[48]
Once pregnancy moves into the second trimester, all the risks of
miscarriage and birth defects occurring drop drastically.
Progesterone has noticeable effects on respiratory physiology,
increasing minute ventilation by 40% in the first trimester.[49]
Second
trimester

By the end of the second trimester, the expanding
uterus has created a visible "baby bump". Although
the breasts have been developing internally since
the beginning of the pregnancy, most of the visible
changes appear after this point.
Weeks 13 to 28 of the pregnancy are called the second
trimester. Most women feel more energized in this period, and
begin to put on weight as the symptoms of morning sickness
subside and eventually fade away. The uterus, the muscular organ
that holds the developing fetus, can expand up to 20 times its
normal size during pregnancy.
Although the
fetus
begins to move and takes a recognizable human shape during the
first trimester, it is not until the second trimester that
movement of the fetus, often referred to as "quickening",
can be felt. This typically happens in the fourth month, more
specifically in the 20th to 21st week, or by the 19th week if
the woman has been pregnant before. However, it is not uncommon
for some women not to feel the fetus move until much later. The
placenta fully functions at this time and the fetus makes
insulin and urinates. The reproductive organs distinguish
the fetus as male or female. During the second trimester, most
women begin to wear
maternity clothes.
Third
trimester

Comparison of growth of the abdomen between 26 weeks
and 40 weeks gestation.
Final weight gain takes place, which is the most weight gain
throughout the pregnancy. The fetus will be growing the most
rapidly during this stage, gaining up to 28 g per day. The
woman's belly will transform in shape as the belly drops due to
the fetus turning in a downward position ready for birth. During
the second trimester, the woman's belly would have been very
upright, whereas in the third trimester it will drop down quite
low, and the woman will be able to lift her belly up and down.
The fetus begins to move regularly, and is felt by the woman.
Fetal movement can become quite strong and be disruptive to the
woman. The woman's
navel
will sometimes become convex, "popping" out, due to her
expanding
abdomen. This period of her pregnancy can be uncomfortable,
causing symptoms like weak bladder control and backache.
Movement of the fetus becomes stronger and more frequent and via
improved brain, eye, and muscle function the fetus is prepared
for ex utero viability. The woman can feel the fetus
"rolling" and it may cause pain or discomfort when it is near
the woman's ribs and spine.

1858 engraving of a pregnant woman showing the fetus
in the womb
There is head engagement in the third trimester, that
is, the fetal head descends into the
pelvic cavity so that only a small part (or none) of it can
be felt abdominally. The perenium and cervix are further
flattened and the head may be felt vaginally.[50]
Head engagement is known colloquially as the baby drop,
and in natural medicine as the lightening because of the
release of pressure on the upper abdomen and renewed ease in
breathing. However, it severely reduces bladder capacity,
increases pressure on the pelvic floor and the rectum, and the
mother may experience the perpetual sensation that the fetus
will "fall out" at any moment.[51]
It is also during the third trimester that maternal activity and
sleep positions may affect fetal development due to restricted
blood flow. For instance, the enlarged uterus may impede blood
flow by compressing the lower pressured
vena cava, with the left lateral laying positions appearing
to providing better oxygenation to the infant.[52]
It is during this time that a baby born
prematurely may survive. The use of modern medical
intensive care technology has greatly increased the
probability of premature babies surviving, and has pushed back
the boundary of viability to much earlier dates than would be
possible without assistance.[53]
In spite of these developments, premature birth remains a major
threat to the fetus, and may result in ill health in later life,
even if the baby survives.
Prenatal
development
Prenatal development is divided into two primary biological
stages. The first is the
embryonic stage, which lasts for about two months. At this
point, the
fetal
stage begins. At the beginning of the fetal stage, the risk
of miscarriage decreases sharply,[54]
and all major structures including the head, brain, hands, feet,
and other organs are present, and they continue to grow and
develop. When the fetal stage commences, a fetus is typically
about 30 mm (1.2 inches) in length, and the heart can be seen
beating via ultrasound; the fetus can be seen making various
involuntary motions at this stage.[55]
Electrical
brain activity is first detected between the 5th and 6th
week of gestation, though this is still considered primitive
neural activity rather than the beginning of conscious thought,
something that develops much later in fetation. Synapses begin
forming at 17 weeks, and at about week 28 begin to multiply at a
rapid pace which continues until 3 to 4 months after birth.[56]
-
Embryo at 4 weeks after fertilization [57]
-
Fetus at 8 weeks after fertilization [58]
-
Fetus at 18 weeks after fertilization [59]
-
Fetus at 38 weeks after fertilization [60]
-
Relative size in 1st month (simplified illustration)
-
Relative size in 3rd month (simplified illustration)
-
Relative size in 5th month (simplified illustration)
-
Relative size in 9th month (simplified illustration)
Physiological changes
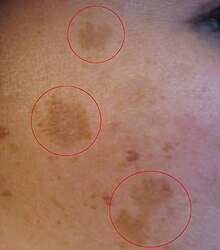
Melasma pigment changes to the face due to
pregnancy
During pregnancy, the woman undergoes many
physiological changes, which are entirely normal, including
cardiovascular,
hematologic,
metabolic,
renal and
respiratory changes that become very important in the event
of complications. The body must change its physiological and
homeostatic mechanisms in pregnancy to ensure the fetus is
provided for. Increases in blood sugar, breathing and cardiac
output are all required. Levels of progesterone and oestrogens
rise continually throughout pregnancy, suppressing the
hypothalamic axis and subsequently the menstrual cycle.
Many women and medical professionals[61][62]
mistakenly think that
breastfeeding causes their breasts to
sag (medically referred to as ptosis),[63]
and as a result some are reluctant to nurse their infants. In
February 2009,
Cheryl Cole told British
Vogue that she hesitated to breastfeed because of the effect
it might have on her breasts. "I want to breastfeed," she said,
"but I've seen what it can do, so I may have to reconsider."[64]
Research shows that breastfeeding is less of a factor than
previously thought. The main risk factors for ptosis are
cigarette smoking, a woman's
body mass index (BMI), her
number of pregnancies, her
breast cup size before pregnancy, and age.[65][66]
Management
Prenatal medical care is the medical and nursing care
recommended for women
before and
during pregnancy. The aim of good prenatal care is to
identify any potential problems early, to prevent them if
possible (through recommendations on adequate nutrition,
exercise, vitamin intake etc.), and to manage problems, possibly
by directing the woman to appropriate specialists, hospitals,
etc. if necessary.
Nutrition
A balanced, nutritious diet is an important aspect of a
healthy pregnancy. Eating a healthy diet, balancing
carbohydrates, fat, and
proteins, and eating a variety of fruits and vegetables,
usually ensures good nutrition. Those whose diets are affected
by health issues, religious requirements, or ethical beliefs may
choose to consult a health professional for specific advice.
Adequate periconceptional
folic acid (also called folate or Vitamin B9)
intake has been shown to decrease the risk of fetal neural tube
defects such as
spina bifida, a serious
birth defect. The neural tube develops during the first 28
days of pregnancy, explaining the necessity to guarantee
adequate periconceptional folate intake.[67][68]
Folate (from folia, leaf) is abundant in
spinach (fresh, frozen, or canned), and is found in
green leafy vegetables e.g. salads, beets, broccoli,
asparagus, citrus fruits and melons, chickpeas (i.e. in the form
of
hummus or
falafel), and
eggs. In the United States and Canada, most wheat products
(flour, noodles) are fortified with folic acid.[69]
DHA omega-3 is a major structural fatty acid in the brain
and retina, and is naturally found in breast milk. It is
important for the woman to consume adequate amounts of DHA
during pregnancy and while nursing to support her well-being and
the health of her infant. Developing infants cannot produce DHA
efficiently, and must receive this vital nutrient from the woman
through the placenta during pregnancy and in breast milk after
birth.[70]
Several
micronutrients are important for the health of the
developing fetus, especially in areas of the world where
insufficient nutrition is prevalent.[71]
In developed areas, such as Western Europe and the United
States, certain nutrients such as
Vitamin D and
calcium, required for bone development, may require
supplementation.[72][73][74]
Dangerous bacteria or parasites may contaminate foods,
including
Listeria and
Toxoplasma gondii. Careful washing of fruits and raw
vegetables may remove these pathogens, as may thoroughly cooking
leftovers, meat, or processed meat. Soft cheeses may contain
Listeria; if milk is raw, the risk may increase. Cat feces
pose a particular risk of
toxoplasmosis. Pregnant women are also more prone to
Salmonella infections from eggs and poultry, which
should be thoroughly cooked. Practicing good hygiene in the
kitchen can reduce these risks.[75]
Weight gain
Caloric intake should be increased to ensure proper
development of the fetus. The amount of weight gained during a
single pregnancy varies. The
Institute of Medicine recommends an overall pregnancy weight
gain for those of normal weight (body
mass index of 18.5–24.9), of 11.3–15.9 kg (25–35 pounds).[76]
Women who are underweight (BMI of less than 18.5), should gain
between 12.7–18 kg (28–40 lbs), while those who are
overweight (BMI of 25–29.9) are advised to gain between
6.8–11.3 kg (15–25 lbs) and those who are
obese (BMI>30) should gain between 5–9 kg (11–20 lbs).[77]
During pregnancy, insufficient or excessive weight gain can
compromise the health of the mother and fetus. Women are
encouraged to choose a healthy diet regardless of pre-pregnancy
weight. Exercise during pregnancy, such as walking and swimming,
is recommended for healthy pregnancies. Exercise has notable
health benefits for both mother and baby, including preventing
excessive weight gain.[78][79]
Medication use
Drugs used during pregnancy can have temporary or permanent
effects on the fetus. Therefore many physicians would prefer not
to prescribe for pregnant women, the major concern being over
teratogenicity of the drugs.
Drugs have been classified into categories A,B,C,D and X
based on the Food and Drug Administration (FDA) rating system to
provide therapeutic guidance based on potential benefits and
fetal risks. Drugs, including some
multivitamins, that have demonstrated no fetal risks after
controlled studies in humans are classified as Category A. On
the other hand drugs like
thalidomide with proven fetal risks that outweigh all
benefits are classified as Category X.[80]
Exposure
to toxins
Various toxins pose a significant hazard to fetuses during
development. A 2011 study found that virtually all U.S. pregnant
women carry multiple chemicals, including some banned since the
1970s, in their bodies. Researchers detected
polychlorinated biphenyls,
organochlorine pesticides,
perfluorinated compounds,
phenols,
polybrominated diphenyl ethers,
phthalates,
polycyclic aromatic hydrocarbons,
perchlorate PBDEs, compounds used as flame retardants, and
dichlorodiphenyltrichloroethane (DDT), a pesticide banned in the
United States in 1972, in the bodies of 99 to 100 percent of the
pregnant women they tested.
Bisphenol A (BPA) was identified in 96 percent of the women
surveyed. Several of the chemicals were at the same
concentrations that have been associated with negative effects
in children from other studies and it is thought that exposure
to multiple chemicals can have a greater impact than exposure to
only one substance.[81][medical
citation needed]
- Alcohol ingestion during pregnancy may cause
fetal alcohol syndrome, a permanent and often
devastating birth-defect syndrome. A number of studies have
shown that light to moderate drinking during pregnancy might
not pose a risk to the fetus, although no amount of alcohol
during pregnancy can be guaranteed to be absolutely safe.[82]
- Children exposed to
prenatal cigarette smoke may experience a wide range of
behavioral, neurological, and physical difficulties.[83]
- Marijuna use during pregnancy is associated with
deficits in language, attention, areas of cognitive
performance, and delinquent behavior in offspring, through
adolescence.[84]
- Elemental
mercury and
methylmercury are two forms of mercury that may pose
risks in pregnancy. Methylmercury, a worldwide contaminant
of seafood and freshwater fish, is known to produce adverse
nervous system effects, especially during brain development.
Eating fish is the main source of mercury exposure in humans
and some fish may contain enough mercury to harm the
developing nervous system of an embryo or fetus, sometimes
leading to learning disabilities.[85]
Mercury is present in many types of fish, but it is mostly
found in certain large fish. The United States
Food and Drug Administration and the
Environmental Protection Agency advise pregnant women
not to eat swordfish, shark, king mackerel and tilefish and
limit consumption of albacore tuna to 6 ounces or less a
week.[85]
- Air pollution can negatively affect a pregnancy
resulting in higher rates of preterm births, growth
restriction, and heart and lung problems in the infant.[86]
- The developing nervous system of the fetus is
particularly vulnerable to lead toxicity. Neurological
toxicity is observed in children of exposed women as a
result of the ability of lead to cross the placental
barrier. A special concern for pregnant women is that some
of the bone lead accumulation is released into the blood
during pregnancy. Several studies have provided evidence
that even low maternal exposures to lead produce
intellectual and behavioral deficits in children.[87]
Sexual
activity
Most women can continue to engage in sexual activity
throughout pregnancy.[88]
Most research suggests that during pregnancy both sexual desire
and frequency of sexual relations decrease.[89][90]
In context of this overall decrease in desire, some studies
indicate a second-trimester increase, preceding a decrease
during the third trimester.[91][92]
Some individuals are sexually attracted to pregnant women (pregnancy
fetishism, also known as
maiesiophilia).
Sex during pregnancy is a low-risk behavior except when the
healthcare provider advises that sexual intercourse be avoided
for particular medical reasons. Otherwise, for a healthy
pregnant woman who is not ill or weak, there is no safe
or right way to have sex during pregnancy: it is enough
to apply the common sense rule that both partners avoid putting
pressure on the uterus, or a partner's full weight on a pregnant
belly.[93]
Exercise
Regular aerobic exercise during pregnancy appears to improve
(or maintain) physical fitness; however, the quality of the
research is poor and the data was insufficient to infer
important risks or benefits for the mother or infant.[94]
The Clinical Practice Obstetrics Committee of Canada
recommends that "All women without contraindications should be
encouraged to participate in aerobic and strength-conditioning
exercises as part of a healthy lifestyle during their
pregnancy". Although an upper level of safe exercise intensity
has not been established, women who were regular exercisers
before pregnancy and who have uncomplicated, healthy pregnancies
should be able to engage in high intensity exercise programs,
such as jogging and aerobics for less than 45 minutes, with no
adverse effects if they are mindful of the possibility that they
may need to increase their energy intake and are careful to not
become overheated. In the absence of either medical or obstetric
complications, they advise an accumulation of 30 minutes a day
of exercise on most if not all days of the week. In general,
participation in a wide range of recreational activities appears
to be safe, with the avoidance of those with a high risk of
falling such as horseback riding or sking or those that carry a
risk of abdominal trauma, such as soccer or hockey.[95]
The American College of Obstetricians and Gynecologists
reports that in the past, the main concerns of exercise in
pregnancy were focused on the fetus and any potential maternal
benefit was thought to be offset by potential risks to the
fetus. However, they write that more recent information suggests
that in the uncomplicated pregnancy, fetal injuries are highly
unlikely. They do, however, list several circumstances when a
woman should contact her health care provider before continuing
with an exercise program. Contraindications include: Vaginal
bleeding,
dyspnea before exertion, dizziness, headache, chest pain,
muscle weakness, preterm labor, decreased fetal movement,
amniotic fluid leakage, and calf pain or swelling (to rule out
thrombophlebitis).
[95]
Complications
Each year, according to the WHO, ill-health as a result of
pregnancy is experienced (sometimes permanently) by more than 20
million women around the world. Furthermore, the "lives of eight
million women are threatened, and more than 500,000 women are
estimated to have died in 1995 as a result of causes related to
pregnancy and childbirth."[96]
Pregnancy poses varying levels of
health risk for women, depending on their medical profile
before pregnancy.
The following are some of the complaints that may occur
during and/or after pregnancy due to the many changes which
pregnancy causes in a woman's body:
-
Pregnancy induced hypertension
-
Anemia[97]
-
Back pain. A particularly common complaint in the third
trimester when the patient's center of gravity has shifted.
-
Carpal tunnel syndrome in between an estimated 21% to
62% of cases, possibly due to edema.[98]
-
Constipation. A complaint that is caused by decreased
bowel mobility secondary to elevated
progesterone (normal in pregnancy), which can lead to
greater absorption of water.
-
Braxton Hicks contractions. Occasional, irregular, and
often painless contractions that occur several times per
day.
-
Edema (swelling). Common complaint in advancing
pregnancy. Caused by compression of the
inferior vena cava (IVC) and pelvic veins by the
uterus leads to increased hydrostatic pressure in lower
extremities.
-
Regurgitation,
heartburn, and
nausea. Common complaints that may be caused by
Gastroesophageal Reflux Disease (GERD); this is
determined by relaxation of the
lower esophageal sphincter (LES) and increased transit
time in the stomach (normal in pregnancy), as well as by
increased intraabdominal pressure, caused by the enlarging
uterus.
-
Haemorrhoids. Complaint that is often noted in advancing
pregnancy. Caused by increased venous stasis and IVC
compression leading to congestion in venous system, along
with increased abdominal pressure secondary to the pregnant
space-occupying uterus and constipation.
-
Pelvic girdle pain.
PGP disorder is complex and multi-factorial and likely
to be represented by a series of sub-groups with different
underlying pain drivers from peripheral or central nervous
system,[99]
altered laxity/stiffness of muscles,[100]
laxity to injury of tendinous/ligamentous structures[101]
to 'mal-adaptive' body mechanics.[99]
Musculo-Skeletal Mechanics involved in
gait and
weightbearing activities can be mild to grossly
impaired. PGP can begin peri or postpartum. There is
pain, instability or dysfunction in the
symphysis pubis and/or
sacroiliac joints.
-
Postpartum depression
-
Postpartum psychosis
-
Round Ligament Pain. Pain experienced when the ligaments
positioned under the uterus stretch and expand to support
the woman's growing uterus
- Thromboembolic disorders. The leading cause of death in
pregnant women in the USA.[102]
-
Increased urinary frequency. A common complaint referred
by the gravida, caused by increased intravascular volume,
elevated GFR (glomerular
filtration rate), and compression of the
bladder by the expanding uterus.
-
Urinary tract infection[103]
-
Varicose veins. Common complaint caused by relaxation of
the venous
smooth muscle and increased intravascular pressure.
-
PUPPP skin disease that develop around the 32nd week.
(Pruritic Urticarial Papules and Plaques of Pregnancy), red
plaques, papules, itchiness around the belly button that
spread all over the body except for the inside of hands and
face.
Ectopic
pregnancy
An ectopic pregnancy is a complication of pregnancy in which
the embryo implants outside the uterine cavity.[104]
With rare exceptions, ectopic pregnancies are not
viable. Most ectopic pregnancies occur in the
Fallopian tube (so-called tubal pregnancies), but
implantation can also occur in the
cervix,
ovaries, and
abdomen. It should be considered in any woman with abdominal
pain or vaginal bleeding who has a positive
pregnancy test. An
ultrasound showing a
gestational sac with fetal heart in a location other than
the uterine cavity is clear evidence of an ectopic pregnancy.
Tubal ectopic pregnancy is the most common cause of maternal
death in the first trimester of pregnancy.[105]
About 1% of pregnancies are in an ectopic location with
implantation not occurring inside of the womb, and of these 98%
occur in the Fallopian tubes.[105]
In a typical ectopic pregnancy, the embryo adheres to the lining
of the fallopian tube and burrows into the tubal lining. Most
commonly this invades blood vessels which causes bleeding
resulting in the expulsion of the implantation from the tube.
Termed "tubal abortions", about half of ectopic pregnancies will
resolve without treatment. The use of
methotrexate treatment for ectopic pregnancy has reduced the
need for surgery, but surgical intervention is still required in
cases where the Fallopian tube has ruptured or is in danger of
doing so. The surgical intervention may be
laparoscopic or through a larger incision, known as a
laparotomy.[106]
A woman who has had a previous ectopic pregnancy is more
likely to have another. The majority of women with ectopic
pregnancies have had
pelvic inflammatory disease or
salpingitis, an inflammation of the fallopian tube. A
history of
gonorrhea or
chlamydia can also cause tubal problems that increase the
risk.
Endometriosis, a condition that causes the tissue that
normally lines the uterus to develop outside the uterus may
slightly increase the incidence of an ectopic. The risk is
increased in women who have unusually shaped fallopian tubes or
tubes which has been damaged, possibly during surgery. Taking
medication to stimulate ovulation increases the risk of ectopic
pregnancy. Although pregnancy is rare when using birth control
pills or an
intrauterine device (IUD), if it does occur, it's more
likely to be ectopic. Although pregnancy is rare after
tubal ligation, if it does occur, it's more likely to be
ectopic.[107]
A recent
meta-analysis of clinical outcomes has shown that cigarette
smoking significantly increases the risk of tubal ectopic
pregnancy.[105]
Concomitant diseases
In addition to
complications of pregnancy that can arise, a woman may have
other diseases or conditions (not directly caused by the
pregnancy) that may become worse or be a potential risk to the
pregnancy.
Epidemiology
The incidence of pregnancy among the female population, as
well as the ages at which it occurs, differ significantly by
country and region, and are often influenced by a multitude of
factors, such as cultural, social and religious norms; access to
contraception; and the prevalence of (higher) education. The
total fertility rate (TFR) in 2013 was estimated to be highest
in
Niger (7.03 children born per woman) and lowest in
Singapore (0.79 children/woman).[109]
In Europe, the average childbearing age has been rising
continuously for some time. In Western, Northern, and Southern
Europe, first-time mothers are on average 26 to 29 years old, up
from 23 to 25 years at the start of the 1970s. In a number of
European countries (Spain), the mean age of women at first
childbirth has now even crossed the 30-year threshold.
This process is not restricted to Europe. Asia, Japan and the
United States are all seeing average age at first birth on the
rise, and increasingly the process is spreading to countries in
the developing world like China, Turkey and Iran. In the U.S.,
the age of first childbirth was 25.4 in 2010.[110]
Society
and culture
In most cultures, pregnant women have a special status in
society and receive particularly gentle care.[111]
At the same time, they are subject to expectations that may
exert great psychological pressure, such as having to produce a
son and heir. In many traditional societies, pregnancy must be
preceded by marriage, on pain of ostracism of mother and
(illegitimate) child.
Depictions of pregnant women can serve as mystically
connotated symbols of fertility. The so-called
Venus of Willendorf with its exaggerated female sexual
characteristics (huge breasts and belly, prominent
mons pubis) has been interpreted as indicative of a
fertility cult in
paleolithic Europe.
Overall, pregnancy is accompanied by numerous customs that
are often subject to ethnological research, often rooted in
traditional medicine or religion. The
baby shower is an example of a modern custom.
Pregnancy is an important topic in
sociology of the family. The prospective child is
preliminarily placed into numerous
social roles such as prospective heir or welfare recipient.
(This may accelerate weddings.) The parents' relationship and
the relation between parents and their surroundings are also
affected.
Arts
Due to the important role of the
Mother of God in Christianity, the Western visual arts have
a long tradition of depictions of pregnancy.[112]
Pregnancy, and especially pregnancy of unmarried women, is
also an important motif in literature. Notable examples include
Hardy's
Tess of the d'Urbervilles and Goethe's
Faust.
Infertility
Modern reproductive medicine offers a choice of measures for
couples who stay childless against their will: fertility
treatment,
artificial insemination and
surrogacy.
Abortion
An abortion is the termination of an embryo or fetus, either
naturally or via medical methods. When done electively, it is
more often done within the first trimester than the second, and
rarely in the third.[54]
Not using contraception, contraceptive failure, poor family
planning or rape can lead to
undesired pregnancies. Legality of socially indicated
abortions varies widely both internationally and through time.
In most countries of Western Europe, abortions during the first
trimester were a criminal offense a few decades ago but have
since been legalized, sometimes subject to mandatory
consultations. In Germany, for example, as of 2009 less than 3%
of abortions had a medical indication.
Legal
protection
Many countries have various legal regulations in place to
protect pregnant women and their children.
Maternity Protection Convention ensures that pregnant women
are exempt from activities such as night shifts or carrying
heavy stocks.
Maternity leave typically provides paid leave from work
during roughly the last trimester of pregnancy and for some time
after birth. Notable extreme cases include Norway (8 months with
full pay) and the United States (no paid leave at all except in
some states). Moreover, many countries have laws against
pregnancy discrimination.
References
-
^
"Embryo definition". MedicineNet, Inc. 27 April
2011.
-
^
"Fetus definition". MedicineNet, Inc. 27 April 2011.
-
^
"Trimester definition". MedicineNet, Inc. 27 April
2011.
-
^
"40% of pregnancies 'unplanned'".
BBC News. 16 March 2004.
-
^
Jayson, Sharon (20 May
2011).
"Unplanned pregnancies in U.S. at 40 percent".
PhysOrg.com.
-
^
K. Joseph Hurt, Matthew W.
Guile, Jessica L. Bienstock, Harold E. Fox, Edward E.
Wallach (eds.).
The Johns Hopkins manual of gynecology and obstetrics
(4th ed.). Philadelphia: Wolters Kluwer Health /
Lippincott Williams & Wilkins. p. 232.
ISBN 9781605474335.
-
^
a
b
"definition of gravida".
The Free Dictionary.
Retrieved 17 January 2008.
-
^
Robinson, Victor,
Ph.C., M.D. (editor) (1939). "Primipara".
The Modern Home Physician, A New Encyclopedia of Medical
Knowledge. WM. H. Wise & Company (New York).,
page 596.
-
^
"Definition of nulligravida".
Merriam-Webster, Incorporated.
Retrieved 9 March 2012.
-
^
"Nulliparous definition". MedicineNet, Inc. 18
November 2000.
-
^
"Fertilization".
Retrieved 28 July 2010.
-
^
a
b
Dr H. Kieler, O.
Axelsson, S. Nilsson, U. Waldenströ (1995). "The length
of human pregnancy as calculated by ultrasonographic
measurement of the fetal biparietal diameter".
Ultrasound in Obstetrics & Gynecology 6 (5):
353–357.
doi:10.1046/j.1469-0705.1995.06050353.x.
PMID 8590208.
-
^
"Pregnancy Due Date Ranges". Spacefem.com.
Retrieved 25 November 2011.
-
^
"Definitions". Saskatchewan Prevention Institute.
Retrieved 16 January 2008.
-
^
Norwitz, MD, PhD, Errol R.
"Postterm Pregnancy (Beyond the Basics)". UpToDate,
Inc. Retrieved 24
August 2012.
-
^
The American College of
Obstetricians and Gynecologists (April 2006).
"What To Expect After Your Due Date". Medem.
Medem, Inc. Retrieved
16 January 2008.
-
^
"Induction of labour – Evidence-based Clinical Guideline
Number 9" (PDF). Royal College of Obstetricians and
Gynaecologists. 2001. Archived from
the original on 30 December 2006.
Retrieved 18 January 2008.
-
^
Stovall, M.D., Thomas G. (23
March 2004).
"Postdate Pregnancy". Durham Obstetrics and
Gynecology. Durham Obstetrics and Gynecology.
Retrieved 18 January 2008.[dead
link]
-
^
"Nonmedically Indicated Early-Term Deliveries".
American College of Obstetricians and Gynecologists.
2013. Retrieved 24
March 2013.
-
^
"Doctors To Pregnant Women: Wait At Least 39 Weeks".
18 July 2011.
Retrieved 20 August 2011.
-
^
"Definition of Premature birth". Medicine.net.
Retrieved 16 January 2008.
-
^
Lama Rimawi, MD (22 September
2006).
"Premature Infant". Disease & Conditions
Encyclopedia. Discovery Communications, LLC.
Retrieved 16 January 2008.
-
^
WHO | Early skin-to-skin contact for mothers and their
healthy newborn infants
-
^
Jenkins, A; Millar, S;
Robins, J (2011 Jul). "Denial of pregnancy: a literature
review and discussion of ethical and legal issues.".
Journal of the Royal Society of Medicine 104
(7): 286–91.
doi:10.1258/jrsm.2011.100376.
PMID 21725094.
-
^
Gabbe, Steven.
Obstetrics : normal and problem pregnancies (6th ed.
ed.). Philadelphia: Elsevier/Saunders. p. 1184.
ISBN 9781437719352.
-
^
"Pregnancy Symptoms".
National Health Service (NHS). 11 March 2010.
Retrieved 11 March 2010.
-
^
a
b
"Early symptoms of pregnancy: What happens right away".
Mayo Clinic. 22 February 2007.
Retrieved 22 August 2007.
-
^
a
b
"Pregnancy Symptoms – Early Signs of Pregnancy :
American Pregnancy Association".
Retrieved 16 January 2008.
-
^
MedlinePlus > Breast pain Update Date: 31 December
2008. Updated by: David C. Dugdale, Susan Storck. Also
reviewed by David Zieve.
-
^
"NHS Pregnancy Planner".
National Health Service (NHS). 19 March 2010.
Retrieved 19 March 2010.
-
^
Qasim SM, Callan C, Choe
JK (1996). "The predictive value of an initial serum
beta human chorionic gonadotropin level for pregnancy
outcome following in vitro fertilization". Journal of
Assisted Reproduction and Genetics 13 (9):
705–8.
doi:10.1007/BF02066422.
PMID 8947817.
-
^
"BestBets: Serum or Urine beta-hCG?".
-
^
Verhaegen, J; Gallos, ID;
van Mello, NM; Abdel-Aziz, M; Takwoingi, Y; Harb, H;
Deeks, JJ; Mol, BW; Coomarasamy, A (2012 Sep 27).
"Accuracy of single progesterone test to predict early
pregnancy outcome in women with pain or bleeding:
meta-analysis of cohort studies.". BMJ (Clinical
research ed.) 345: e6077.
doi:10.1136/bmj.e6077.
PMC 3460254.
PMID 23045257.
-
^
Nguyen, T.H.; et al.
(1999).
"Evaluation of ultrasound-estimated date of delivery in
17 450 spontaneous singleton births: do we need to
modify Naegele's rule?" (abstract). Ultrasound in
Obstetrics and Gynecology 14 (1): 23–28.
doi:10.1046/j.1469-0705.1999.14010023.x.
PMID 10461334.
Retrieved 18 August 2007.
-
^
Whitworth, M; Bricker, L;
Neilson, JP; Dowswell, T (2010 Apr 14). "Ultrasound for
fetal assessment in early pregnancy.". In Whitworth,
Melissa. Cochrane database of systematic reviews
(Online) (4): CD007058.
doi:10.1002/14651858.CD007058.pub2.
PMID 20393955.
-
^
a
b
"Screening for Ultrasonography in Pregnancy".
U.S. Preventive Services Task Force.
Retrieved 6 March 2013.
-
^
Bricker, L; Neilson, JP;
Dowswell, T (2008 Oct 8). "Routine ultrasound in late
pregnancy (after 24 weeks' gestation).". In Bricker,
Leanne. Cochrane database of systematic reviews
(Online) (4): CD001451.
doi:10.1002/14651858.CD001451.pub3.
PMID 18843617.
-
^
Dimitrova V, Markov D,
Dimitrov R (2007). "[3D and 4D ultrasonography in
obstetrics]". Akush Ginekol (Sofiia) (in
Bulgarian) 46 (2): 31–40.
PMID 17469450.
-
^
Sheiner E, Hackmon R,
Shoham-Vardi I, et al. (2007). "A comparison
between acoustic output indices in 2D and 3D/4D
ultrasound in obstetrics". Ultrasound Obstet Gynecol
29 (3): 326–8.
doi:10.1002/uog.3933.
PMID 17265534.
-
^
Rados C (January–February
2004).
"FDA Cautions Against Ultrasound 'Keepsake' Images".
FDA Consumer Magazine. Archived from
the original on 13 May 2009.
Retrieved 28 February 2012.
-
^
Kempley R (9 August 2003).
"The Grin Before They Bear It; Peek-a-Boo: Prenatal
Portraits for the Ultrasound Set". Washington
Post.
-
^
trimester. CollinsDictionary.com. Collins English
Dictionary – Complete & Unabridged 11th Edition.
Retrieved 26 November 2012.
-
^
thefreedictionary.com > trimester Citing:
- The American
Heritage® Dictionary of the English Language, Fourth
Edition, copyright 2000
-
^
Cunningham, et al., (2010). Williams Textbook of
Obstetrics, chapter 8.
-
^
"Early pregnancy symptoms: Morning sickness, fatigue and
other common symptoms".
Retrieved 2011.
-
^
"Pregnancy video". Channel 4. 2008.
Retrieved 22 January 2009.
- ^
a
b
"Pregnancy week by week".
Retrieved 28 July 2010.
-
^
"Pregnancy Week by week Symptoms".
Retrieved 28 July 2010.
-
^
Campbell, LA; Klocke, RA
(2001 Apr). "Implications for the pregnant patient.".
American journal of respiratory and critical care
medicine 163 (5): 1051–4.
doi:10.1164/ajrccm.163.5.16353.
PMID 11316633.
-
^
"Starting labour". pregnancy-bliss.co.uk.
Retrieved 14 January 2009.
-
^
"Lightening During Pregnancy as an Early Sign of Labor".
Giving Birth Naturally.
Retrieved 22 August 2010.
-
^
Stacey, T; Thompson, JM;
Mitchell, EA; Ekeroma, AJ; Zuccollo, JM; McCowan, LM
(2011 Jun 14).
"Association between maternal sleep practices and risk
of late stillbirth: a case-control study.". BMJ
(Clinical research ed.) 342: d3403.
doi:10.1136/bmj.d3403.
PMC 3114953.
PMID 21673002.
-
^
Iams, JD; Romero, R;
Culhane, JF; Goldenberg, RL (2008 Jan 12). "Primary,
secondary, and tertiary interventions to reduce the
morbidity and mortality of preterm birth.". Lancet
371 (9607): 164–75.
doi:10.1016/S0140-6736(08)60108-7.
PMID 18191687.
-
^
a
b
•
Q&A: Miscarriage. (6 August 2002). BBC News.
Retrieved 2007-04-22: "The risk of miscarriage lessens
as the pregnancy progresses. It decreases dramatically
after the 8th week."
•
Lennart Nilsson,
A Child is Born 91 (1990): at eight weeks, "the
danger of a miscarriage … diminishes sharply."
• "Women's
Health Information", Hearthstone Communications
Limited: "The risk of miscarriage decreases dramatically
after the 8th week as the weeks go by." Retrieved
2007-04-22.
-
^
Kalverboer, edited by Alex
F.; Gramsbergen, Albert (2001).
Brain and behaviour in human development.
Dordrecht: Kluwer. pp. 415–418.
ISBN 9780792369431.
-
^
Illes, ed. by Judy (2008).
Neuroethics : defining the issues in theory,
practice, and policy (Repr. ed.). Oxford: Oxford
University Press. p. 142.
ISBN 9780198567219.
-
^
3D Pregnancy (Image from gestational age of 6
weeks). Retrieved 2007-08-28. A rotatable 3D version of
this photo is available
here, and a sketch is available
here.
-
^
3D Pregnancy (Image from gestational age of 10
weeks). Retrieved 2007-08-28. A rotatable 3D version of
this photo is available
here, and a sketch is available
here.
-
^
3D Pregnancy (Image from gestational age of 20
weeks). Retrieved 2007-08-28. A rotatable 3D version of
this photo is available
here, and a sketch is available
here.
-
^
3D Pregnancy (Image from gestational age of 40
weeks). Retrieved 2007-08-28. A rotatable 3D version of
this photo is available
here, and a sketch is available
here.
-
^
Lauersen, Niels H.; Stukane,
Eileen (1998). The Complete Book of Breast Care
(1st Trade Paperback ed.). New York: Fawcett
Columbine/Ballantine.
ISBN 978-0-449-91241-6.
-
^
"Breast Sagging".
Retrieved 2 February 2012.
-
^
"Sagging Breasts". Channel 4. 2009.
Retrieved 3 February 2012.
-
^
Jay, Elizabeth (13 February
2009).
"Will breastfeeding leave you with a little less lift?".
Retrieved 2 February 2012.
-
^
Thompson, Andrea (2 November
2007).
"Breastfeeding Does Not Make Breasts Sag, Study
Suggests". LiveScience.com.
Retrieved 2 February 2012.
-
^
Campolongo, Marianne (5
December 2007).
"What Causes Sagging Breasts?".
Retrieved 26 January 2012.
-
^
Klusmann A, Heinrich B,
Stöpler H, Gärtner J, Mayatepek E, Von Kries R (2005).
"A decreasing rate of neural tube defects following the
recommendations for periconceptional folic acid
supplementation". Acta Paediatr. 94
(11): 1538–42.
doi:10.1080/08035250500340396.
PMID 16303691.
Retrieved 20 January 2008.
-
^
Stevenson RE, Allen WP,
Pai GS, Best R, Seaver LH, Dean J, Thompson S (2000).
"Decline in prevalence of neural tube defects in a
high-risk region of the United States". Pediatrics
106 (4): 677–83.
doi:10.1542/peds.106.4.677.
PMID 11015508.
-
^
Centers for Disease
Control and Prevention (CDC) (2008). "Use of supplements
containing folic acid among women of childbearing
age—United States, 2007". MMWR Morb. Mortal. Wkly.
Rep. 57 (1): 5–8.
PMID 18185493.
-
^
Salem N, Jr; Litman, B;
Kim, HY; Gawrisch, K (2001 Sep). "Mechanisms of action
of docosahexaenoic acid in the nervous system.".
Lipids 36 (9): 945–59.
doi:10.1007/s11745-001-0805-6.
PMID 11724467.
-
^
Haider BA, Bhutta ZA
(2006). "Multiple-micronutrient supplementation for
women during pregnancy". In Bhutta, Zulfiqar A.
Cochrane Database Syst Rev (4): CD004905.
doi:10.1002/14651858.CD004905.pub2.
PMID 17054223.
-
^
Theobald HE (2007).
"Eating for pregnancy and breast-feeding". J Fam
Health Care 17 (2): 45–9.
PMID 17476978.
-
^
Basile LA, Taylor SN,
Wagner CL, Quinones L, Hollis BW (2007). "Neonatal
vitamin D status at birth at latitude 32 degrees 72':
evidence of deficiency". J Perinatol 27
(9): 568–71.
doi:10.1038/sj.jp.7211796.
PMID 17625571.
-
^
Kuoppala T, Tuimala R,
Parviainen M, Koskinen T, Ala-Houhala M (1986). "Serum
levels of vitamin D metabolites, calcium, phosphorus,
magnesium and alkaline phosphatase in Finnish women
throughout pregnancy and in cord serum at delivery".
Hum Nutr Clin Nutr 40 (4): 287–93.
PMID 3488981.
-
^
Tarlow, MJ (1994 Aug).
"Epidemiology of neonatal infections.". The Journal
of antimicrobial chemotherapy. 34 Suppl A: 43–52.
PMID 7844073.
-
^
"Weight Gain During Pregnancy: Reexaminging the
Guidelines, Report Brief". Institute of Medicine.
Retrieved 29 July 2010.
-
^
American College of
Obstetricians and Gynecologists (January 2013). "Weight
Gain During Pregnancy". Obstet Gynecol 121
(1): 210–2.
doi:10.1097/01.AOG.0000425668.87506.4c.
PMID 23262962.
-
^
"Pregnancy and Exercise: Baby Let's Move!". Mayo
Clinic. Retrieved
29 July 2010.
-
^
WADSWORTH, P (1 May
2007).
"The Benefits of Exercise in Pregnancy". The
Journal for Nurse Practitioners 3 (5):
333–339.
doi:10.1016/j.nurpra.2007.03.002.
-
^
Shaji, Reena (13 January
2009).
"Drugs in pregnancy and teratogenicity". LifeHugger.
-
^
"99% of pregnant women in US test positive for multiple
chemicals including banned ones, study suggests".
Sciencedaily.com. 14 January 2011.
doi:10.1289/ehp.1002727.
Retrieved 25 November 2011.
-
^
Ornoy, A; Ergaz, Z (2010
Feb).
"Alcohol abuse in pregnant women: effects on the fetus
and newborn, mode of action and maternal treatment.".
International journal of environmental research and
public health 7 (2): 364–79.
doi:10.3390/ijerph7020364.
PMC 2872283.
PMID 20616979.
-
^
Hackshaw, A; Rodeck, C;
Boniface, S (2011 Sep-Oct).
"Maternal smoking in pregnancy and birth defects: a
systematic review based on 173 687 malformed cases and
11.7 million controls.". Human reproduction
update 17 (5): 589–604.
doi:10.1093/humupd/dmr022.
PMC 3156888.
PMID 21747128.
-
^
Irner, TB (2012).
"Substance exposure in utero and developmental
consequences in adolescence: a systematic review.".
Child neuropsychology : a journal on normal and abnormal
development in childhood and adolescence 18
(6): 521–49.
doi:10.1080/09297049.2011.628309.
PMID 22114955.
-
^
a
b
Abelsohn, A;
Vanderlinden, LD; Scott, F; Archbold, JA; Brown, TL
(2011 Jan).
"Healthy fish consumption and reduced mercury exposure:
counseling women in their reproductive years.".
Canadian family physician Medecin de famille canadien
57 (1): 26–30.
PMC 3024155.
PMID 21322285.
-
^
Backes, CH; Nelin, T;
Gorr, MW; Wold, LE (2013 Jan 10).
"Early life exposure to air pollution: how bad is it?".
Toxicology letters 216 (1): 47–53.
doi:10.1016/j.toxlet.2012.11.007.
PMC 3527658.
PMID 23164674.
-
^
"Chapter 1, Lead-based Paint Hazards, 98–112".
Cdc.gov. Retrieved 25
November 2011.
-
^
Sex during pregnancy: What's OK, what's not -
MayoClinic.com
-
^
M.P. Bermudez; A.I.
Sanchez, G. Buela-Casal (2001).
"Influence of the Gestation Period on Sexual Desire".
Psychology in Spain 5 (1): 14–16.
-
^
Wing Yee Fok; Louis
Yik-Si Chan, Pong Mo Yuen (October 2005). "Sexual
behavior and activity in Chinese pregnant women".
Acta Obstetricia et Gynecologica Scandinavica 84
(10): 934–938.
doi:10.1111/j.0001-6349.2005.00743.x.
PMID 16167907.
-
^
Reamy K; White SE,
Daniell WC, Le Vine ES (June 1982). "Sexuality and
pregnancy. A prospective study". J Reprod Med.
27 (6): 321–7.
PMID 7120209.
-
^
Malarewicz A, Szymkiewicz
J, Rogala J (September 2006). "[Sexuality of pregnant
women]". Ginekol. Pol. (in Polish) 77 (9):
733–9.
PMID 17219804.
-
^
Cory Silverberg (19 September
2011).
"Pregnancy Sex Positions: ideas for comfortable sex
positions during pregnancy". About.com Guide.
-
^
Kramer, MS; McDonald, SW
(19 July 2006).
"Aerobic exercise for women during pregnancy". In
Kramer, Michael S. Cochrane database of systematic
reviews (Online) 3 (3): CD000180.
doi:10.1002/14651858.CD000180.pub2.
PMID 16855953.
-
^
a
b
Artal, R; O'Toole, M
(2003 Feb).
"Guidelines of the American College of Obstetricians and
Gynecologists for exercise during pregnancy and the
postpartum period.". British journal of sports
medicine 37 (1): 6–12; discussion 12.
doi:10.1136/bjsm.37.1.6.
PMC 1724598.
PMID 12547738.
-
^
"Reproductive Health and Research Publications: Making
Pregnancy Safer". World Health Organization Regional
Office for South-East Asia. 2009.
Retrieved 7 December 2009.
-
^
Merck.
"Pregnancy complicated by disease". Merck Manual,
Home Health Handbook. Merck Sharp & Dohme.
-
^
Mondelli,M.; Rossi,S.; Monti,E.; Aprile,I.;
Caliandro,P.; Pazzaglia,C.; Romano,C.; Padua,L. (2007)
Long term follow-up of carpal tunnel syndrome during
pregnancy: a cohort study and review of the literature.
Electromyogr Clin Neurophysiol. 2007 Sep;47(6):259–71.
-
^
a
b
O'Sullivan, Peter B.;
Beales, Darren J. (May 2007).
"Diagnosis and classification of pelvic girdle pain
disorders—Part 1: A mechanism based approach within a
biopsychosocial framework". Manual Therapy
12 (2): 86–97.
doi:10.1016/j.math.2007.02.001.
PMID 17449432.
-
^ European
guidelines for the diagnosis and treatment of pelvic
girdle pain.Eur Spine J. 2008 Feb 8 Vleeming A, Albert
HB, Ostgaard HC, Sturesson B, Stuge B.
-
^ Possible
role of the long dorsal sacroiliac ligament in women
with peripartum pelvic pain. Acta Obstetricia et
Gynecologica Scandinavica Volume 81 Issue 5 Page
430-436, May 2002, Andry Vleeming, Haitze J. de Vries,
Jan M. A Mens, Jan-Paul van Wingerden
-
^
C. Blackwell, Sean (December
2008).
"Thromboembolic Disorders During Pregnancy". Merck
Sharp & Dohme Corp.
-
^
Merck.
"Urinary tract infections during pregnancy".
Merck Manual Home Health Handbook.
-
^
Page EW, Villee CA, Villee
DB. Human Reproduction, 2nd Edition. W. B.
Saunders, Philadelphia, 1976. p. 211.
ISBN 0-7216-7042-3.
-
^
a
b
c
Shaw, J. L. V.; Dey, S.
K., Critchley, H. O. D., Horne, A. W. (January 2010).
"Current knowledge of the aetiology of human tubal
ectopic pregnancy". Human Reproduction Update
16 (4): 432–444.
doi:10.1093/humupd/dmp057.
PMC 2880914.
PMID 20071358.
-
^
Laparoscopic Ectopic Pregnancy Surgery - Powered by
World Laparoscopy Hospital
-
^
Ectopic pregnancy: Risk factors - MayoClinic.com
-
^
a
b
Health Care Guideline: Routine Prenatal Care. Fourteenth
Edition. By the Institute for Clinical Systems
Improvement. July 2010.
-
^
https://www.cia.gov/library/publications/the-world-factbook/rankorder/2127rank.html
-
^
http://www.cdc.gov/nchs/data/nvsr/nvsr61/nvsr61_01.pdf
-
^
Womack, Mari (2010).
The anthropology of health and healing..
Plymouth: AltaMira Press. p. 133.
ISBN 978-0-7591-1044-1.
-
^
Rossi, Timothy Verdon ;
captions by Filippo (2005).
Mary in western art. New York: In Association
with Hudson Hills Press. p. 106.
ISBN 0-9712981-9-X.
External links

|
blog comments powered by
|
|
DA INGLESE A ITALIANO
Inserire
nella casella Traduci la parola
INGLESE e cliccare
Go.
DA ITALIANO A INGLESE
Impostare INGLESE anziché italiano e
ripetere la procedura descritta.
|
Acupuncture
Artificial skin
Bipolar disorder
British Medical Association
Cardiac surgery
Cryosurgery
Delirium tremens
Diabetes mellitus
Doctor of Medicine
Drug design
Eating disorder
Emergency department
Epidemiology
Foodborne illness
Foot
Health
Heart
Hip replacement
Hospital
Human anatomy
Human skin
Hypnosis
International Classification of Diseases
Jet lag
List of medical schools in the United Kingdom
Liver
Medical drama
Medical ultrasonography
Medicare (United States)
Medicine
Mount Sinai Hospital
Noble Prize in Physiology or Medicine
Nursing
Obstetrics
Optometry
Palliative care
Paramedic
Phytotherapy
Preventive medicine
Prognosis
Prosthesis
Radiology
Rhytidectomy (Facelift)
Scalpel
Sildenafil
Tinnitus
Tooth brushing
Trauma center
Vital signs
World Health Organization
|